Nearly one in three fever patients who opted for Fever package tested positive for serious infections
In India, fever is brushed off casually. “Just viral”. “Wait it out”. “Paracetamol and rest.”
But between 2023 and 2025, diagnostic data tells a far more alarming story, one that turns casual reassurance into a dangerous oversight. Behind what appears to be an ordinary fever, a significant proportion of patients were diagnosed with infections that required medical intervention, from dengue and malaria to typhoid and other illnesses. The numbers challenge a deeply rooted cultural habit: self-diagnose, self-medicate, and wait.
Serious Infections Are More Common Than You Think
Among 1.08 lakh people who chose a comprehensive Fever Package, nearly 1 in 3 tested positive for a major infection, dengue, typhoid, malaria,leptospirosis or chikungunya. Typhoid alone showed up in nearly one in five patients (18.1%), with dengue close behind (about 1 in 7, 14.4%), along with malaria, chikungunya and leptospirosis, further adding to the burden.
These results make one thing evident: a meaningful proportion of fever cases are not vague or self-limiting, but have clearly defined infectious causes. Structured testing transforms uncertainty into clarity and clarity into timely action.

Co-infections were strikingly common in Fever Package Patients
Almost 10% of infection-positive patients (2982 cases) weren’t battling a single illness. They had co-infections. In nearly 70% of these instances, the co-infection involved dengue and typhoid. The presence of dual infections adds a layer of complexity to diagnosis and treatment. When illnesses share similar early clinical features but demand different therapeutic approaches, identifying only one may not provide the complete clinical picture.
This is where a “wait and watch” approach reveals its limitations. In the setting of co-infection, delays in comprehensive evaluation can mean delayed or incomplete treatment.
Shifting Fever Trends (2023–2025) in Fever Package Testing
India’s fever landscape is changing. Over three years, the dominant infections within fever cases have shifted noticeably. Dengue positivity nearly halved, while malaria doubled, quietly resurging despite its lower overall base. Typhoid and chikungunya spiked in 2024, then eased but did not disappear.
(Chikungunya: 3% → 5.1% → 2%, Typhoid: 17.2% → 20.2% → 16.3%, Dengue: 18.6% → 15.2% → 8.5%, and Malaria: 0.5% → 0.9% → 1.1%)
These movements underscore a simple reality that infectious disease patterns are not linear. They rise, recede, and re-emerge within short spans of time. What guided clinical suspicion last year may not apply this year. In an increasingly fluid epidemiological landscape, adaptive surveillance and sustained diagnostic vigilance must supersede assumption based management.
Fever and Organ Stress: Insights from Patients
Low platelets (thrombocytopenia) were observed in 27% of fever patients, nearly double the 15% seen in non-fever cases. The contrast was particularly stark in malaria-positive patients, where nearly 8 in 10 experienced a platelet drop, versus just 0.04 in 10 in malaria-negative cases. Dengue-positive patients also showed significant platelet reductions, with 37% affected, versus 15% in dengue-negative cases. These findings quantify the hematological perturbations associated with specific infections and demonstrate that laboratory indices can detect systemic involvement beyond the clinical manifestation of fever alone.
Liver enzyme abnormalities were widespread. More than half of all fever patients (56%) had elevated SGOT and 37% had elevated SGPT, versus 42% and 26% in non-fever patients respectively. Fever patients showed striking liver stress compared with non-fever cases in Dengue (SGOT 71% vs 42%, SGPT 44% vs 27%), Malaria (SGOT 56% vs 43%, SGPT 43% vs 28%), Leptospirosis (SGPT 48% vs 34%). These findings demonstrate that liver involvement is a common and clinically relevant feature across multiple infectious diseases. Monitoring liver function therefore becomes an important component of comprehensive fever evaluation.
Fever Package Insights by Gender: Typhoid Up in Females, Malaria Up in Males
Fever positivity was slightly higher in females (32% vs 29%), driven largely by typhoid (21% vs 15%). In contrast, malaria struck men more than twice as often as women (1.1% vs 0.5%). Gender-specific trends in infections point to differences in exposure and risk. Awareness of these patterns can inform better screening and prevention strategies.
Fever Has Geography: Mapping Risks in the Fever Package Testing
In states like Bihar, Haryana, Karnataka, Punjab and UP, over a third of fever patients were diagnosed with serious infections, underlining regionalvariations. Dengue remains dominant in Haryana and Bihar, typhoid is most prevalent in Bihar, Punjab, and Delhi, chikungunya peaks in Punjab and Andhra Pradesh, while malaria clusters in Maharashtra and Gujarat. These patterns show that fever is rarely a one-size-fits-all symptom and awareness of state-specific patterns allow clinicians to prioritize testing, anticipate complications, and intervene promptly.
Disease Burden from Standalone Fever Testing in India
Standalone fever testing across 2.59 lakh patients from 2023 to 2025 recorded an overall positivity of 22.6%, highlighting a substantial infectious disease burden.
. Dengue led in testing volume (1.44 lakh tests; 16.6% positivity).
. Typhoid was second (1.15 lakh tests; 22.7% positivity), showing higher positivity relative to testing volume.
. Malaria had low detection despite extensive testing (90K+ tests; 1.6% positivity).
. Chikungunya, tested in fewer patients (27.9K tests), recorded high positivity (23%).
These patterns indicate that even targeted testing for individual infections can detect a substantial burden of disease. However, relying solely on standalone tests may miss co-infections or less obvious infections, highlighting the importance of comprehensive panels for a more complete understanding of the infectious landscape and timely clinical decision-making.
Geographic Trends from Standalone Fever Testing (2023–2025)
From 2023–2025, Jammu & Kashmir, Bihar, and Punjab recorded the highest overall fever positivity (38%, 34%, 31%). Dengue was concentrated in J&K, Punjab, and Bihar, while typhoid peaked in Bihar and Maharashtra. Chikungunya surged in Punjab and Telangana, and Malaria positivity was highest in Goa and Maharashtra. These patterns provide a clear snapshot of regional infection hotspots based on standalone fever testing, showing where particular pathogens were most active during this period.
The Calendar of Fever
Dengue Trends By Month (2023–2025)
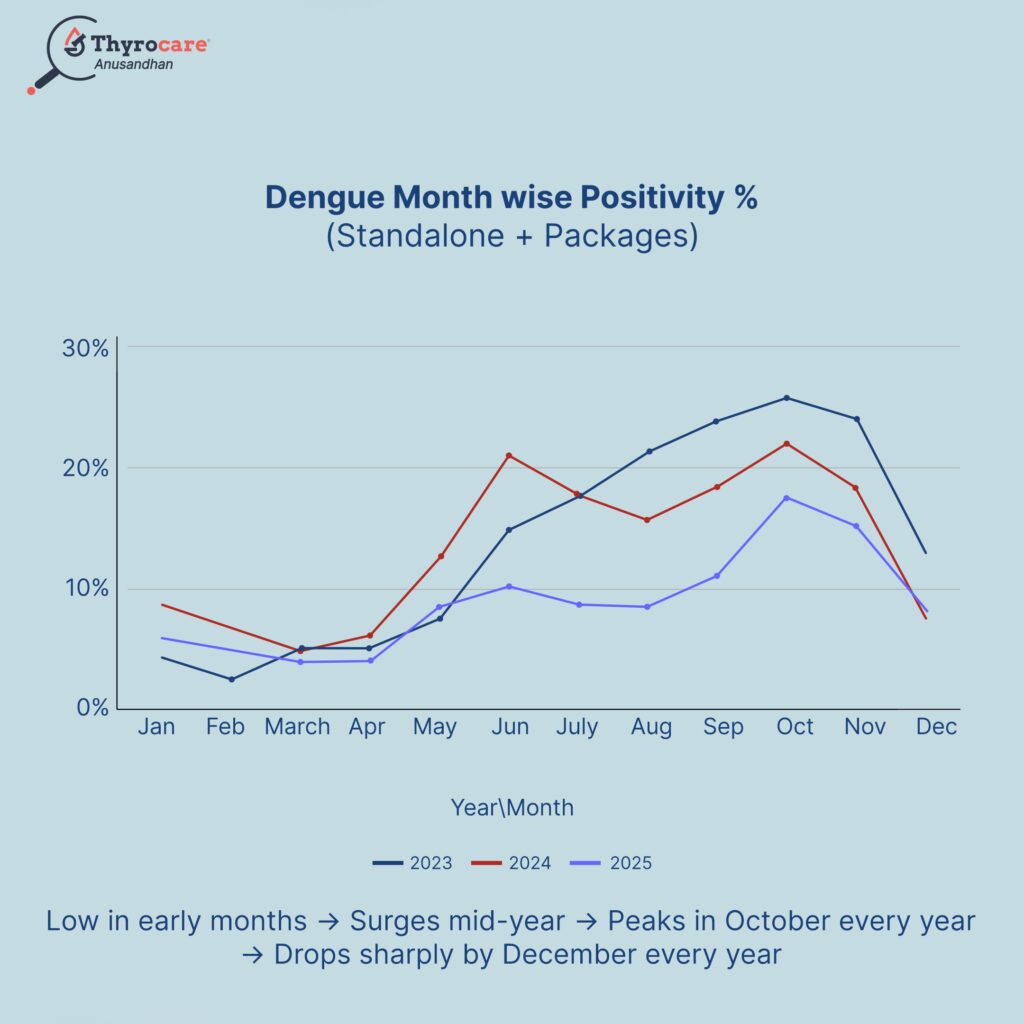
Dengue positivity is low in early months, surges mid-year in June–July (2023–24) with an earlier May surge in 2025. October is consistently the peak month, while positivity drops sharply by December each year.
Typhoid Trends By Month (2023–2025)
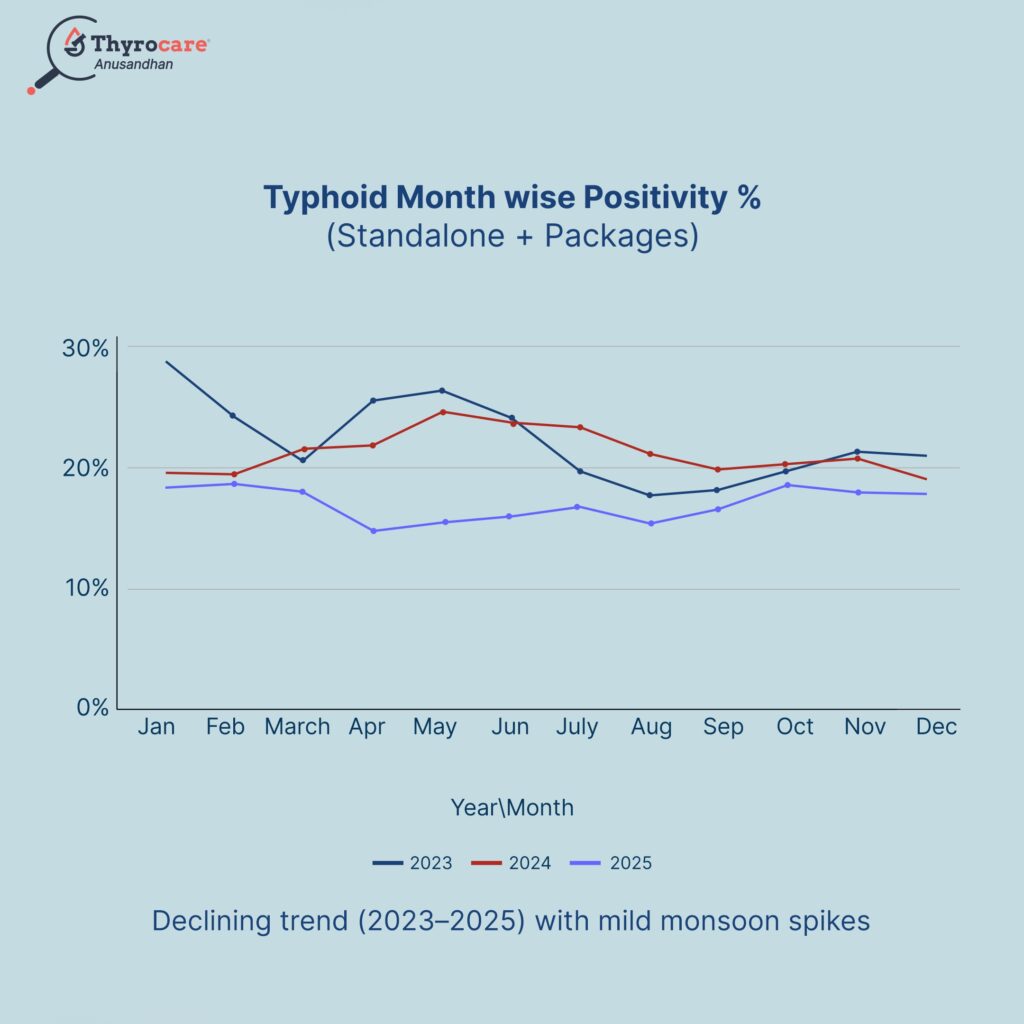
Typhoid positivity has steadily declined from the high, volatile levels of 2023 to a more stable 2024, reaching its lowest in 2025. All years show a mild monsoon rise, but 2025 remains consistently below previous levels, signaling a reduced overall burden.
Chikungunya Trends By Month (2023–2025)
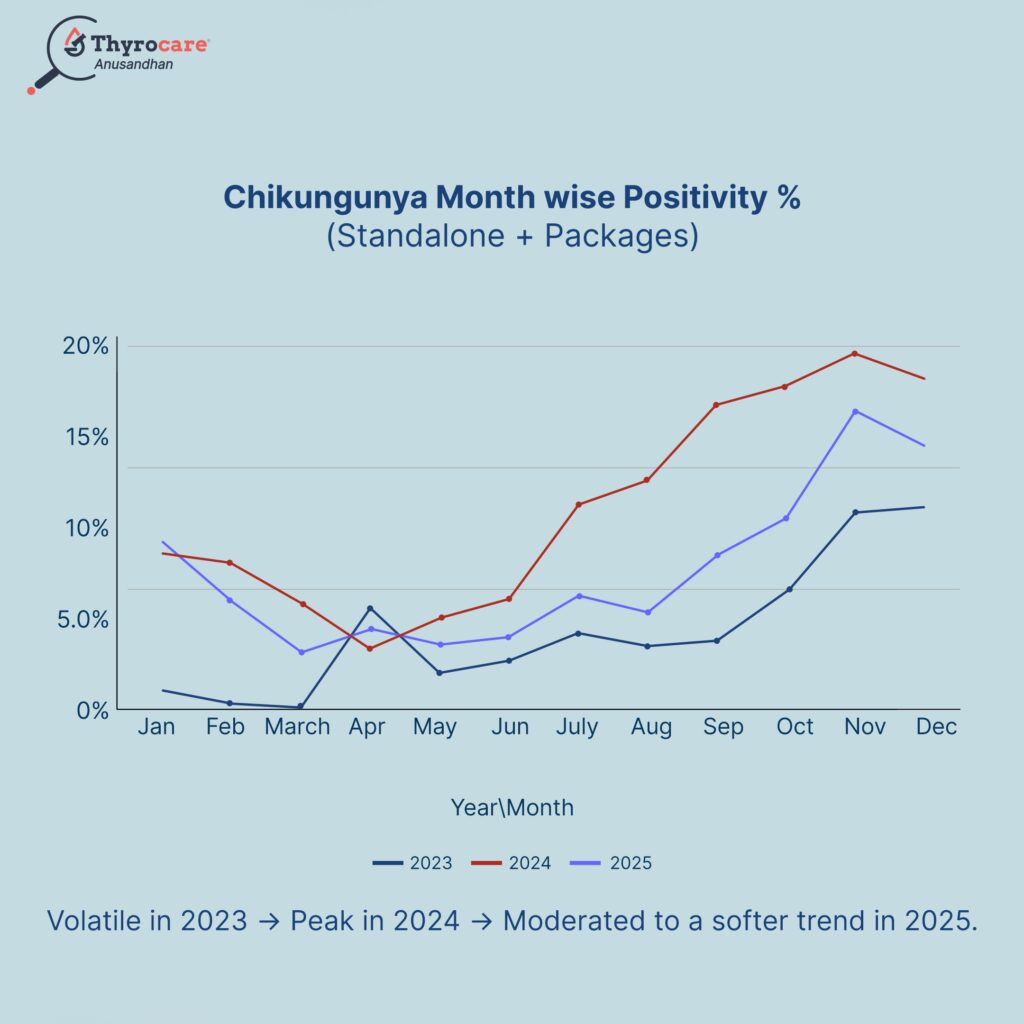
Chikungunya positivity peaked in 2024 with a strong year-end surge, while 2025 has a steadier moderate rise and 2023 remains lower and more fluctuating.
Malaria Trends By Month (2023–2025)
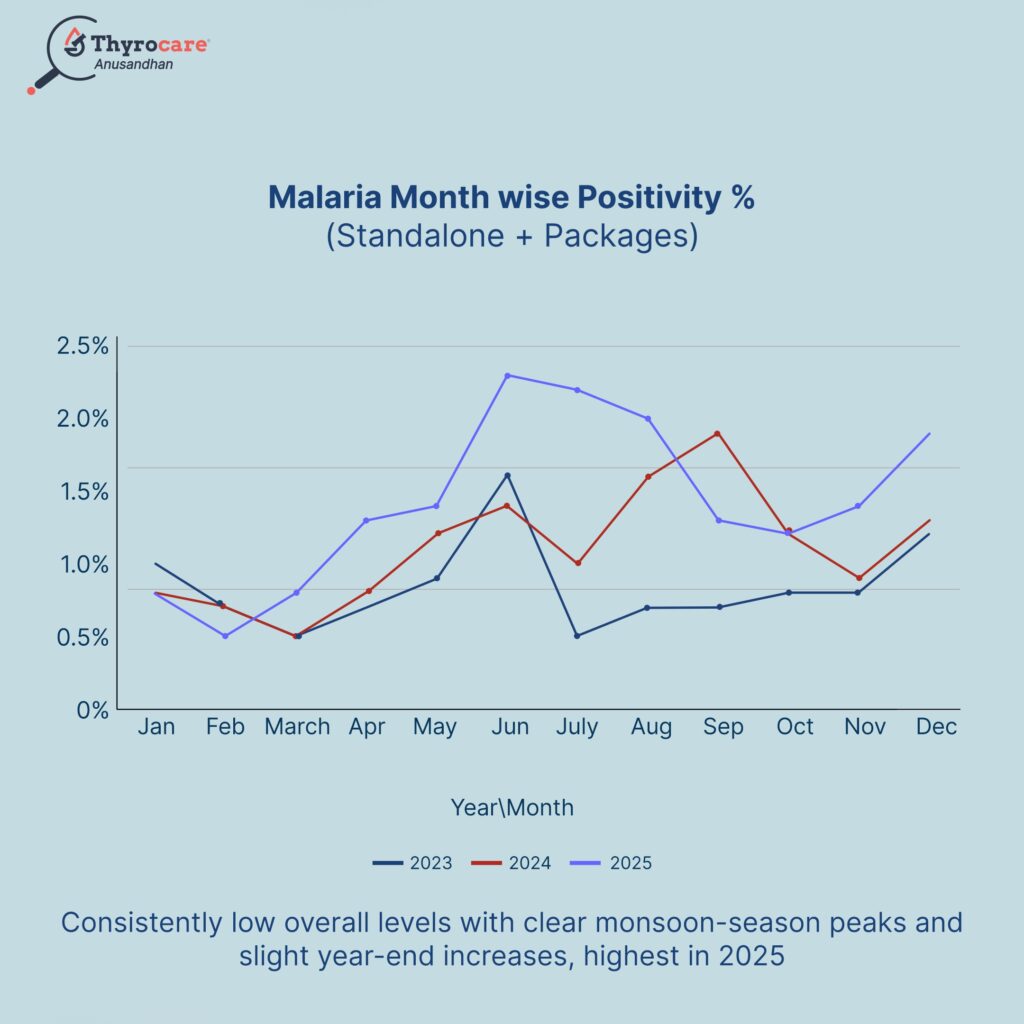
Malaria positivity stayed low (<2.5%) across all three years, peaking mid-year (May–September) during the monsoon. 2025 shows relatively higher positivity, while 2023–24 exhibit comparatively lower and more moderate transmission patterns.
Heat Maps for Typhoid & Dengue Transmission – Overall – (Standalone + Package)
Driving the majority of serious cases, dengue and typhoid heat maps show where India’s fever hits hardest.
Dengue transmission 2023 – 2025 (Standalone + Packages)
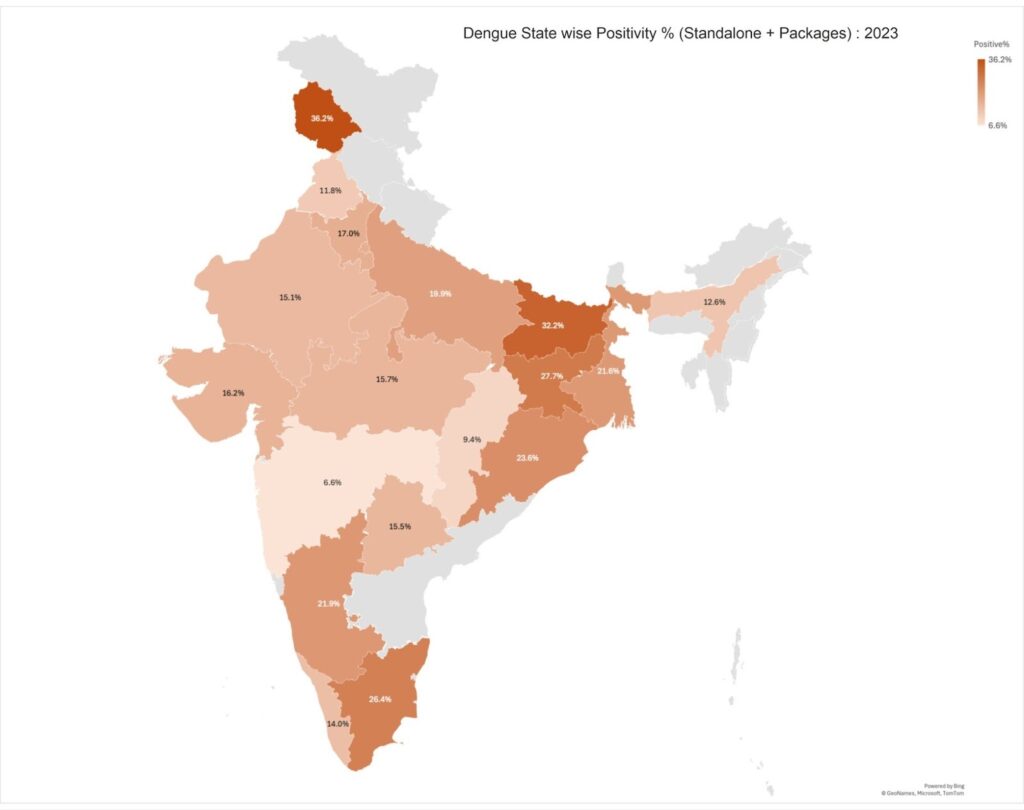
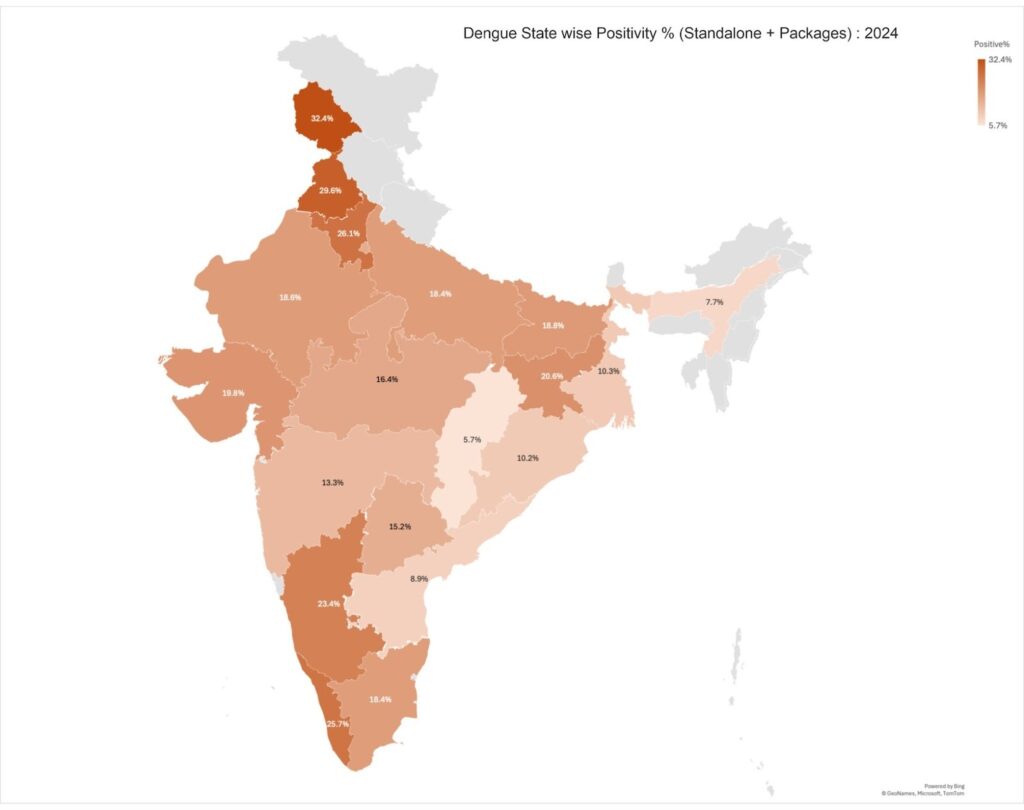
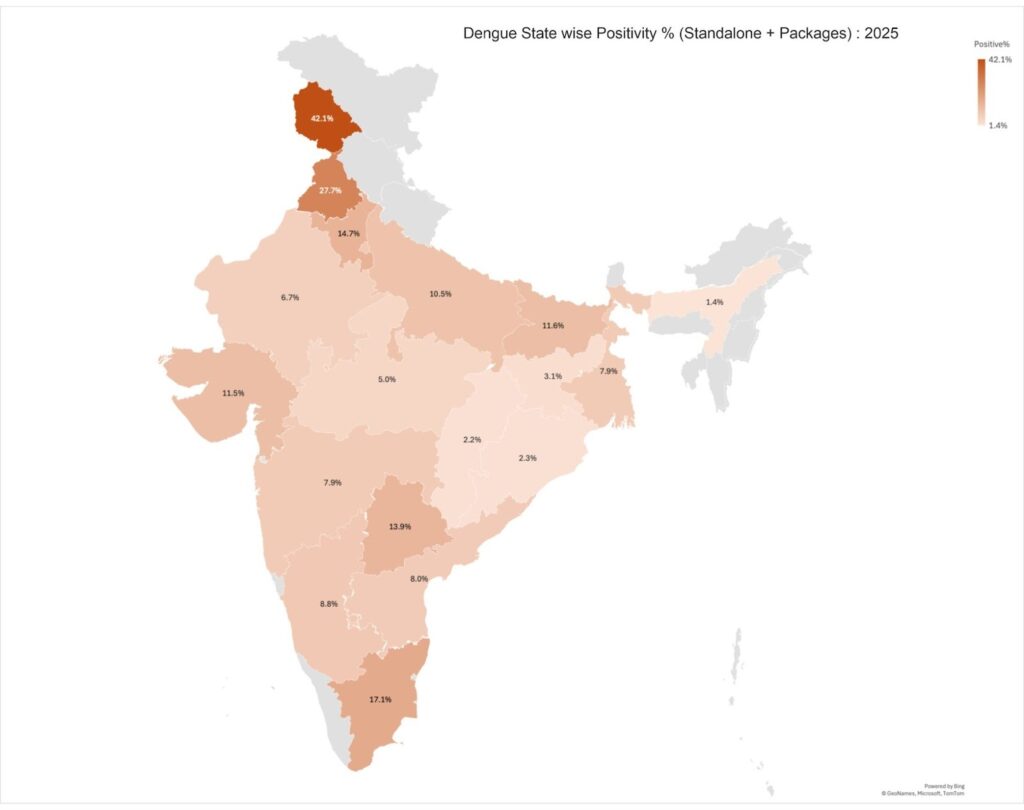
Dengue transmission demonstrates significant inter-state variability, with certain regions consistently recording elevated positivity rates over the three-year period. Analysis from 2023 to 2025 shows a downward trend in most states, potentially reflecting improvements in surveillance and vector-control efforts.
Typhoid transmission 2023 – 2025 (Standalone + Packages)
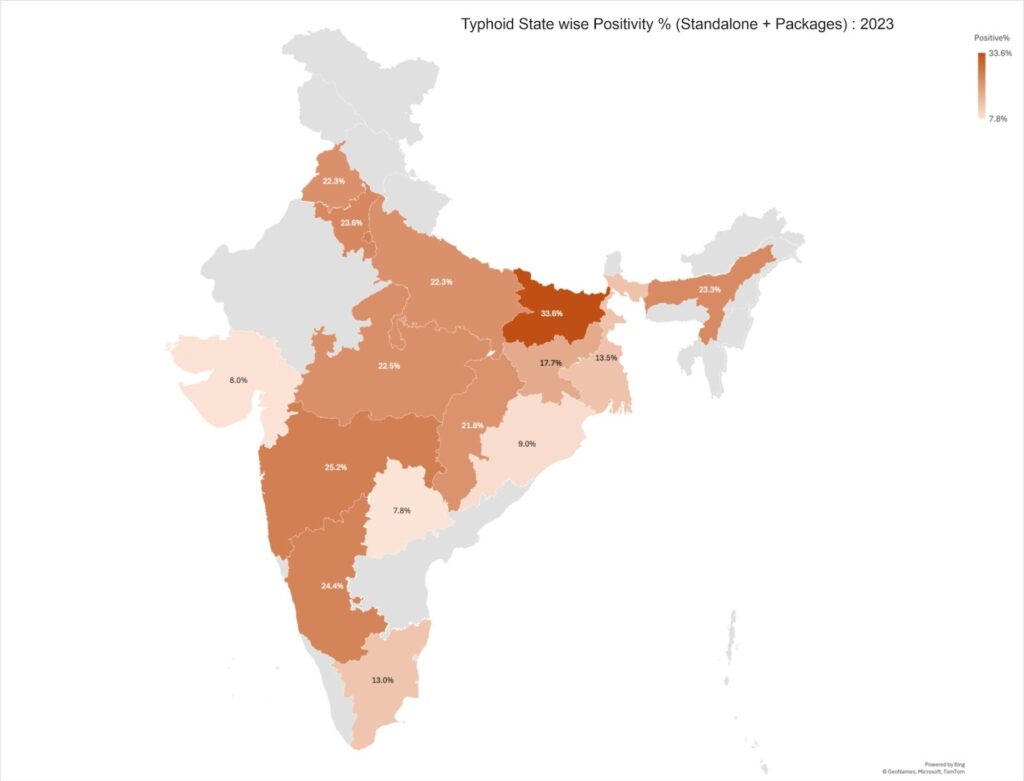
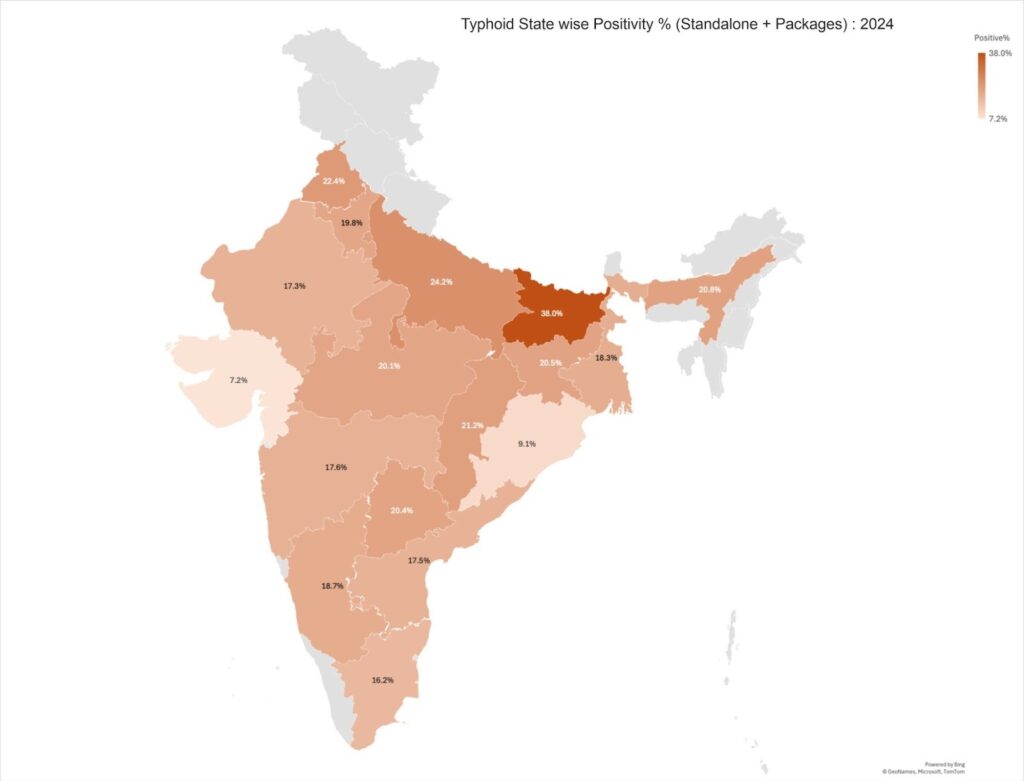
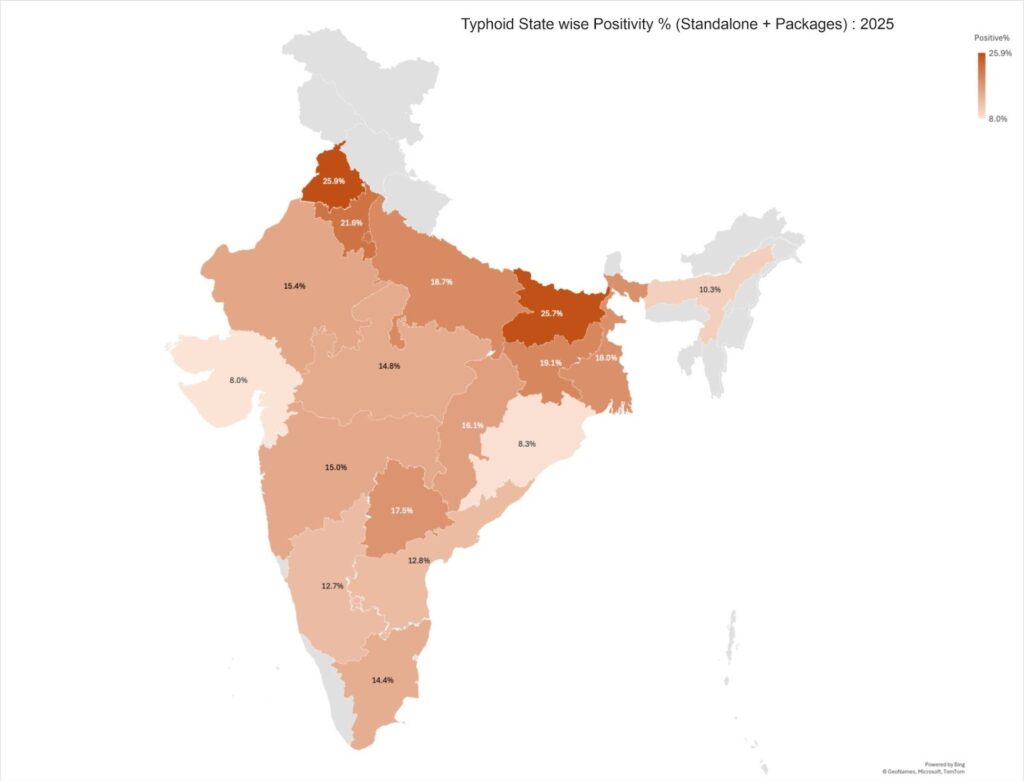
Typhoid positivity trends vary across regions, with some geographies reporting consistently higher transmission rates than others. However, most states demonstrate a gradual decline from 2023 to 2025, indicating an overall reduction in typhoid transmission nationally.
Disclaimer: States with under 500 tests are excluded to prevent low testing skew in geographic trends and heat maps.
Fever is rarely just a fleeting symptom; it is often a window into the body’s deeper battles.
Rahul Guha, MD & CEO of Thyrocare, said, “Recognising fever as a critical signal empowers patients and clinicians alike to act decisively. It shifts care from reactive treatment to timely and informed intervention. Ultimately, early evaluation, supported by data-driven insights, remains one of the most effective ways to navigate India’s evolving and unpredictable infectious disease landscape.”
Dr. Preet Kaur – Chief Scientific Officer, Thyrocare said, “Data from 2023 to 2025 shows that a significant number of patients carry serious infections, sometimes more than one at a time, revealing patterns that simple assumptions cannot capture. Beyond the visible rise in temperature, laboratory markers highlight hidden stress on organs, from drops in platelet counts to elevated liver enzymes, underscoring that fever is a systemic signal, not an isolated event.”
Infection trends shift with geography, gender, season, and year, showing that what was true yesterday may no longer apply today. Certain infections dominate in some regions, while others resurge unexpectedly, making local awareness crucial. Co-infections add further complexity, as illnesses with similar early symptoms can demand very different treatments. Standalone tests may miss these overlaps, emphasizing the value of comprehensive diagnostic panels. Relying on guesswork or delayed evaluation is no longer a safe option. Prompt, thorough assessment enables targeted intervention and prevents complications from escalating.




